Human papillomavirus (HPV) is one of the most common viruses globally — nearly everyone will be infected at some point in their life. Although in around 90 % of cases the virus is cleared spontaneously by the immune system, it can nonetheless cause various complications such as genital warts and cancer.
What makes it more challenging is that some complications may manifest 10 to 20 years after infection, which often leads to inadequate awareness or delayed preventive actions. Therefore, understanding HPV clearly can greatly improve lifestyle choices and preventive measures.
In this article, we provide a clear overview of HPV: what it is, its symptoms, how it spreads, differences in men and women, health consequences, the link with cancer, how it is diagnosed, how to prevent it, and how it is treated. If you are concerned about HPV or genital warts, stay with us until the end.
What is HPV (Human Papillomavirus)?
HPV (Human Papillomavirus) is a very common sexually transmitted infection (STI). According to the World Health Organization (WHO), it is a small non-enveloped double-stranded DNA virus that infects skin or mucosal cells.
There are more than 100 known HPV types; about 60 of them produce skin warts and around 40 types infect the genital region (resulting in genital warts).
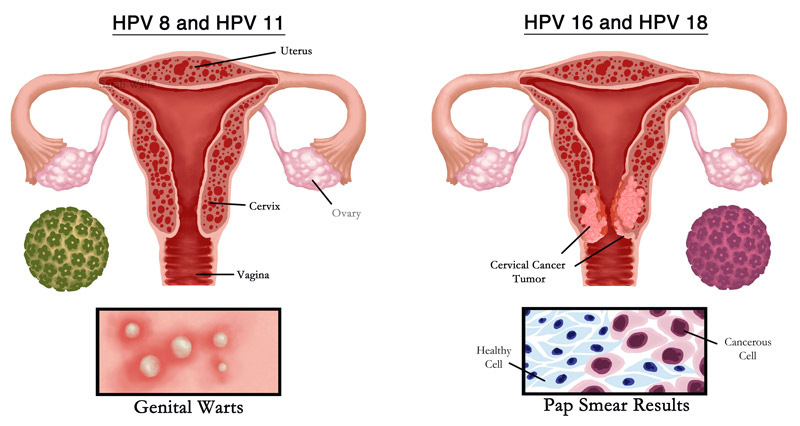
Some types are low-risk (for instance types 6 and 11) that tend to cause benign genital warts. Others are high-risk (for example types 16, 18, 31, 33, 45, 52, 58) which are responsible for the majority of cervical cancers and other carcinomas.
What are the Symptoms of HPV?
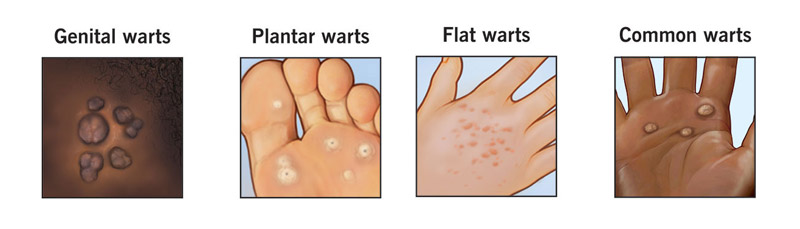
In most cases, HPV infections cause no symptoms at all. If symptoms do appear, the most common sign is genital warts — small cauliflower-like bumps on the genital skin.
It is important to realize that having genital warts does not necessarily lead to cancer. Only a subset of HPV types (the high-risk ones) have that potential. So, spotting a genital wart is a trigger to consult a healthcare provider — but not an immediate sign of cancer.
How is HPV Transmitted?
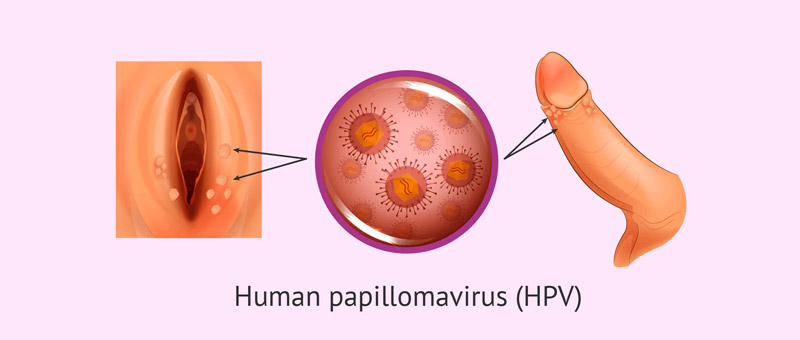
HPV spreads through skin-to-skin contact, especially in the genital region. It does not necessarily require penetrative sex: genital-genital, oral-genital or anal-genital contact can transmit the virus.
Because the virus can infect skin surfaces that are not covered by condoms, using a condom does not guarantee full protection.
Although sexual transmission is the common path, non-sexual skin contact theoretically can play a role. But sexual contact remains the major route.
HPV in Men and Women
Contrary to a common misconception, HPV affects both men and women. While women may face higher risks of certain complications (e.g., cervical cancer), men are certainly not immune.
In men, HPV may lead to genital warts and — in rare cases — penile, anal or throat cancers.
In women, HPV is the main cause of cervical cancer. For example, in the U.S., thousands of women each year develop cervical cancer attributed to HPV.
Therefore preventive efforts apply to all genders.
Health Complications of HPV
While many HPV infections resolve spontaneously (often within 1-2 years) without causing problems, there are potential complications:
- Genital warts (caused by low-risk HPV types) which may be uncomfortable and socially distressing.
- Persistent infection by high-risk HPV types may cause cell changes (dysplasia) in affected tissues which over many years may progress to cancer.
Because such progression can take many years (even 10-20 years) before cancer appears, regular screening and monitoring are very important.
The cancers linked to HPV include cervical cancer, anal cancer, penile cancer, vulvar/vaginal cancer and some head and neck cancers.
HPV and Cancer
It’s crucial to emphasise that HPV ≠ cancer. Having HPV does not mean you will get cancer. Most people infected with HPV will never develop cancer.
However:
- High-risk HPV types (e.g., 16 and 18) are associated with approximately 70 % of cervical cancers globally.
- The process from HPV infection to cancer may span a decade or two if unchecked.
Therefore early detection, screening and preventive measures are key.
How is HPV Diagnosed?
Because many HPV infections are silent (no symptoms), diagnosis often relies on screening rather than symptom-based testing.
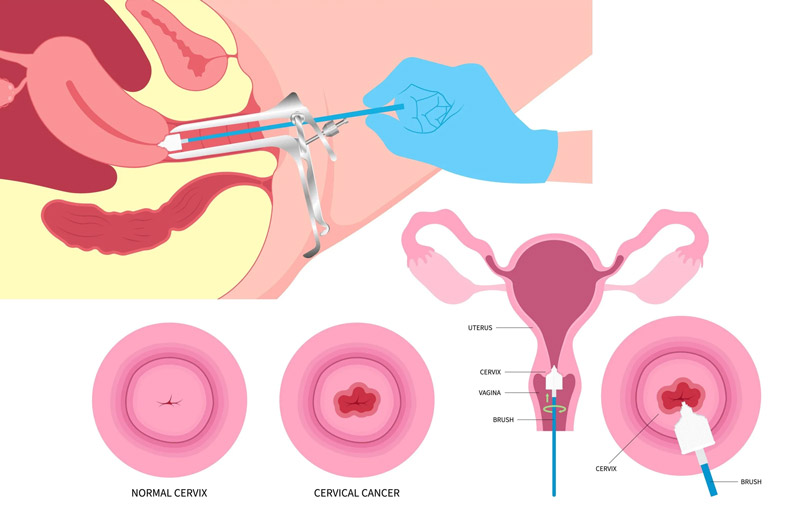
- For women: The Pap smear (Pap test) is widely used to detect abnormal cervical cells and can act as a proxy for HPV-related cell changes.
- There are also HPV DNA tests that detect high-risk HPV types.
- For men: There is no approved routine HPV test.
If genital warts are observed, that in itself may prompt further examination. But absence of warts does not rule out HPV.
How to Prevent HPV
Prevention strategies include:
- Vaccination: Vaccines against HPV are highly effective in preventing infection by high-risk and low-risk types.
- Screening: Regular cervical screening (Pap tests and HPV tests) for women helps detect cell changes early.
- Safer sexual practices: Using condoms, reducing number of sexual partners, and delaying sexual debut help reduce risk — though do not provide absolute protection.
Combining vaccination + screening + safer sex is the best preventive approach.
How is HPV Treated?
Currently there is no cure that completely removes HPV from the body.
However:
- Visible lesions such as warts or abnormal tissue can be treated (e.g., cryotherapy, LEEP, laser, topical medications).
- Treatment of these complications improves outcomes, but does not guarantee elimination of HPV from body.
Hence the emphasis remains on prevention and monitoring.
Conclusion
HPV is one of the most common viruses worldwide — almost everyone will encounter it. Yet, lack of awareness and delayed actions mean many people remain vulnerable to complications. In this article, we reviewed what HPV is, its symptoms, transmission, how it affects men and women, health risks, the cancer link, diagnosis, prevention and treatment.
If you still have questions or doubts about HPV, genital warts or related concerns, please consult a specialist and ask for screening or vaccination as appropriate.



